Osteoarthrosis is a common disorder of synovial joints and is characterized by cartilage degeneration with secondary changes in the adjacent bone.
Osteoarthrosis is seen most often in older patients.
The joints most commonly affected in osteoarthrosis are the knee, hip, hands, and the first metatarsophalangeal joint.
There can be involvement of other joints such as the ankle, wrist and shoulder is uncommon, and suggests a secondary cause for it.
Although osteoarthrosis may be present in many joints, symptoms are usually evident only in one or two joints.
The three main symptoms are pain, morning stiffness, and a tendency for the affected joint to go along with immobility.
Treatment includes rest; weight loss; physiotherapy; aids such as canes, shoe lifts, and elastic knee supports; and judicious use of anti-inflammatory medications.

Table of Contents
ToggleCauses of Osteoarthrosis
There are many causes linked to Osteoarthrosis that is mentioned below. Following conditions can cause osteoarthrosis
1. Primary Osteoarthrosis
Unknown
2. Secondary Osteoarthrosis
- Anatomical abnormalities
- Congenital hip dysplasia
- Avascular necrosis
- Slipped femoral epiphysis
- Fractures Trauma Neuropathic disorders (Charcot’s joints)
- Syringomyelia
- Diabetes mellitus
- Syphilis Hypermobility disorders
3. Metabolic disorders
- Ochronosis
- Hemochromatosis
- Gout
- Chondrocalcinosis
- Hemophilia
- Paget’s disease
- Wilson’s disease
4. Inflammatory disorders
- Rheumatoid arthritis
- Seronegative arthropathies
- Septic arthritis
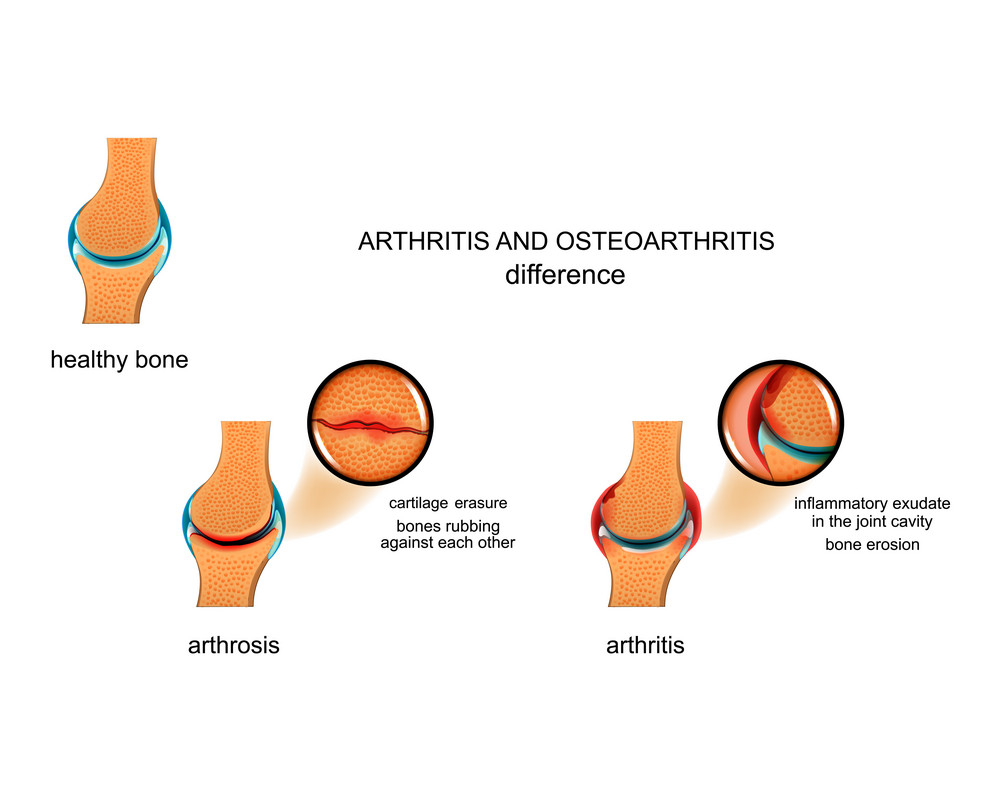
Types of Osteoarthrosis
The types of Osteoarthrosis are mentioned below
1. Primary Osteoarthrosis:-
Primary Osteoarthrosis is further classified depending on factors :-
A. Osteoarthrosis due to aging:-
As osteoarthrosis is most common in old people, it is evident that the disease is part of the aging process.
It seems that the ability of articular cartilage to resist fatigue-testing diminishes with age, and that aging cartilage might represent an accumulation, over time, due to mechanical injuries.
B. Obesity
It is not clear if obesity is associated with an increased prevalence of osteoarthrosis in non-weight bearing joints, it is evident that obesity is associated with increased osteoarthrosis of the knee, but not of the hip.
The majority of obese people exhibit various deformities of the knee, presumably because of attempts to bring the feet under the center of gravity when the thighs are separated by fat.
High weight results in increased load on the medial compartment of the knee, with subsequent degeneration of the knee joints.
C. Heredity Genetic factors
This factor plays a complex role in osteoarthrosis. There are some genetic diseases for example congenital hip disease that can change the joint structure so there is secondary degeneration in the joints.
Also, some inborn errors of metabolism can result in metabolic changes in cartilage leading to secondary degenerative change like in ochronosis.
The changes in normal joints which predispose people to osteoarthrosis are genetically determined, it is observed that Heberden’s nodes depend upon a single autosomal gene, sex influenced to be dominant in females and recessive in males.
The gene frequency analysis suggests three percent of the population are homozygous affected, 27% are heterozygous, and 70%o are homozygous normal. 30% of women over age 45 have evidence of Heberden’s nodes, whereas only three percent of men are affected.
2. Secondary Osteoarthrosis:-
It is when osteoarthrosis is probably not a single disease, but rather a common response to a variety of metabolic, anatomical, and physiological conditions.
Altered congruity of joint surfaces and subtle incongruity of the articulating surfaces of joints may account for many cases of osteoarthrosis in the hip and knee.
The majority of cases of ‘primary’ osteoarthrosis of the hip may well be secondary to a developmental abnormality that occurs during growth the commonest cause is congenital hip dysplasia, which accounts for at least 25% of osteoarthrosis of the hip in older people. Other causes are Legg-Perthes disease and slipped femoral epiphysis.
Similarly, many reasons for ‘primary’ osteoarthrosis of the knee are secondary to fractures of the femoral condyles, ligamentous laxity resulting in instability, chronic patellar dislocation, and severe valgus and varus deformities.
Inflammatory joint disease Inflammatory diseases such as rheumatoid arthritis and septic joints can lead to extensive cartilage damage and secondary osteoarthrosis.
Initial cartilage damage is probably initially enzymatic, with a breakdown of cartilage by enzymes released from inflamed synovium or leukocytes within the joint cavity.
Deposition diseases of cartilage like a variety of metabolic diseases result in the deposition in the cartilage of materials that are noxious and damage the chondrocytes or cartilage matrix itself. These metabolic disease conditions include hemochromatosis, Wilson’s disease, gout, calcium pyrophosphate dehydrate (CPPD) crystal deposition disease, and ochronosis.
Symptoms of Osteoarthrosis
The symptoms of osteoarthrosis include:-
Pain
The affected joints might hurt during or after movement, pain may arise from several sources, that include increased venous pressure in subchondral bone, trabecular microfractures, the elevation of the periosteum by osteophytes, due to ligamentous strain as a result of joint laxity, aggravated by muscle weakness; distension of the joint capsule with effusion and synovitis.
Morning stiffness
Joint stiffness is seen upon awakening or after being inactive.
Morning stiffness is usually shortlived and does not have the duration and intensity that is seen in rheumatoid arthritis
Tenderness
Your joint might feel tender on applying light pressure on or near it. Physical signs include tenderness of the joint, especially with active synovitis or capsular thickening.
Joint effusions are common and usually are due to phagocytosis of cartilage debris by synovial cells, and traumatic effusion as a result of shortness.
The flexibility of joints will be lost
The patient might not be able to move the joint through its full range of motion.
Joint friction sensation
Patients might feel a grating sensation when you use the joint, and one might hear crackling.
Complications of Osteoarthrosis
Osteoarthrosis is a degenerative disease when left untreated can also lead to the following complications-
Chronic joint pains, these joint pain, and stiffness can become severe enough to make daily tasks difficult.
One can get into depression and sleep disturbances can result from the pain and disability of osteoarthritis.
Risk Factors For Osteoarthrosis
- Now Some of the common risk factors are
Older age
- The risk of osteoarthritis increases with age, it is commonly observed in 40 years and above age group people.
Gender
- Women are more likely to develop osteoarthritis, though it isn’t clear why genetic factors are evident.
Obesity
Extra body weight contributes to osteoarthritis in several ways, and the more one weighs, the greater the risk. Increased weight adds stress to weight-bearing joints, like hips and knees. Fat tissue produces proteins that can cause harmful inflammation in and around the joints.
Joint injuries
Injuries, such as those that occur when playing sports or from an accident, can increase the risk of osteoarthritis.
Even injuries that occurred many years ago and have healed can increase your risk of osteoarthrosis.
Repeated stress on the joint
If a job or a sport one plays places repetitive stress on a joint, that joint might eventually develop osteoarthrosis.
Genetics
Some people inherit a tendency to develop osteoarthrosis, it is more common in women.
Deformities of bones
Some people are born with malformed joints or defective cartilage.
Metabolic diseases
These include diabetes and a condition in which the body has too much iron – hemochromatosis.
Diagnosis of Osteoarthrosis
Doctors will usually make a diagnosis during the physical exam, your doctor will check your affected joint for tenderness, swelling, redness, and flexibility. To get pictures of the affected joint, your doctor might recommend:
X-ray
Usually, cartilage doesn’t show up on X-ray images, but cartilage loss is revealed by a narrowing of the space between the bones in the joint. An X-ray can also show bone spurs around a joint very clearly.
Magnetic resonance imaging (MRI)
MRI uses radio waves and a strong magnetic field to produce detailed images of bone and soft tissues, including cartilage. It is useful in the complex case of osteoarthrosis
Lab tests
Analyzing the blood or joint fluid can help to confirm the diagnosis.
Blood tests
There is no specific blood test for osteoarthrosis, but certain tests can help rule out other causes of joint pain, such as rheumatoid arthritis and gout.
Joint fluid analysis
The doctor might use a needle to draw fluid from an affected joint. The fluid is then tested for inflammation to determine whether the pain is caused by gout or infection rather than osteoarthrosis.
Prevention and Management of Osteoarthrosis
Osteoarthritis cannot be reversed, but treatments can reduce pain and help you move better.
Medications
Medications that can help relieve osteoarthrosis symptoms, mainly the pain, include:
Acetaminophen
Acetaminophen has been shown its effectiveness in people with osteoarthrosis who have mild to moderate pain.
Nonsteroidal Anti-inflammatory Drugs (NSAIDs) Tests: –
Over the counter NSAIDs, such as ibuprofen, Advil, Motrin IB, and naproxen sodium -Aleve, taken at the recommended doses, typically relieve osteoarthrosis pain.
Therapy
Physical therapy
A physical therapist can teach a few exercises to strengthen the muscles around your joint, increase flexibility and reduce pain.
Regular gentle exercise that one does on own, such as swimming or walking, can be equally effective.
Occupational therapy
An occupational therapist can guide ways to do everyday tasks without putting extra stress on your already painful joint.
For example, a toothbrush with a large grip could make brushing teeth easier if you have osteoarthrosis in your hands.
A bench in your shower could help relieve the pain of standing if you have knee osteoarthrosis.
Transcutaneous electrical nerve stimulation (TENS):
This uses a low-voltage electrical current to relieve pain and will provide short-term relief for some people with knee and hip osteoarthrosis.
Surgical and other procedures
If conservative treatments fail, then one might want to consider procedures such as:
Cortisone injections:
Injections of a corticosteroid into the joint might relieve pain for a few weeks. The doctor numbs the area around your joint, then places a needle into the space within the joint and injects medication.
The number of cortisone injections is limited to three or four, as the medication can worsen joint damage over time.
Lubrication injections
Injections of hyaluronic acid might relieve pain by providing some cushioning in the knee.
Hyaluronic acid is similar to a component normally found in your joint fluid.
Realigning bones
If osteoarthrosis has damaged one side of the knee more than the other, an osteotomy may be helpful.
In a knee osteotomy, a surgeon cuts across the bone above or below the knee, and then removes or adds a wedge of bone.
This shifts your body weight away from the worn-out and damaged part of the knee.
Joint replacement
In joint replacement surgery, the surgeon removes your damaged joint surfaces and replaces them with plastic and metal parts.
Surgical risks include infections and blood clots.
The artificial joints may wear out or can become loose and might eventually need to be replaced again.
Lifestyle and home remedies
Simple lifestyle changes often provide relief from the frequency of recurrence doctor may also recommend making changes to everyday habits, like:
- One should start taking iron, vitamin B12, folic acid, and vitamin C supplements
- One should aim at reaching or maintaining a moderate body weight
- One should avoid or limit alcohol intake if intake is in excess
- One needs to manage sugar levels in case of diabetes or metabolic syndrome properly if suffering from these conditions.
- One should eat a healthful, balanced diet, including dietary sources of iron, like dark leafy green vegetables, beans and pulses, and dried fruits.
Best Homeopathic Medicines for Osteoarthrosis
Homeopathy is a holistic system of medicine that treats not only the symptoms of the disease but also the man who is suffering from the disease.
So, after a complete detailed history of present and past disease and considering the family history also, a drug is prescribed which will be based on the individualization of every patient.
In mild cases, improvement can be seen within weeks, whereas severe cases will take a longer time. Along with homeopathic medicine, the patients have to follow a healthy regimen for optimum results.
Now, let’s go through some of the homeopathic medicines that can help in tailbone pain. Some of the best homeopathic medicines for the treatment of tailbone pain are mentioned below.
- Symphytum officinalis
- Bryonia
- Rhus tox
- Ruta Graveolen
- Calcarea phosphorica
- Calcarea flourica
- Aurum Metallicum
- Fluoric acid
- Phosphoric acid
- Phosphorus
1. Symphytum Officinalis – For Osteoarthrosis due to fracture
This is a great remedy, especially in the case of an aftereffect of fracture, it favors the production of callus.
It is indicated when the periosteal pains after wounds have healed or irritability at the point of fracture.
It helps in reducing the pricking pains in the joints.
Dosage and potency: 30c, 200c 4 globules (pills) dissolved in half a cup of water 2 times a day for 15 days.
2. Bryonia Alba – For Osteoarthrosis worse from motion
Bryonia alba is indicated for osteoarthrosis which is worse from motion all joints and parts of the body are ameliorated by absolute rest and pressure.
It is used when all complaints develop slowly and have an insidious beginning.
It is indicated for dropsical effusions into the serous and synovial membranes resulting in pleurisy and osteoarthrosis.
Dosage and potency: 200c, 4 globes in half cup of water thrice a day till the symptom disappear.
3. Rhus Toxicodendron – For Osteoarthrosis with the stiffness of joints
Rhus Tox is a wonderful remedy for people who have osteoarthrosis with severe restlessness, the patient cannot stay in one place and must change position frequently.
It is used for osteoarthrosis with great rigidity, stiffness, lameness, and pain experienced on first moving the joints after rest and waking up in the morning.
It is indicated when there is aggravation at night and damp rainy weather rest and heat relieves in general.
It is prescribed for osteoarthrosis when symptoms are worse in the open air and humid weather, and desire for cold milk, sweets, beer, oysters, and an aversion to meat and liquor.
Dosage and potency: 30c, 200c, take 4 drops of dilution in half a cup of water twice a day, till the improvement is seen.
4. Ruta Graveolen – For osteoarthrosis due to mechanical injuries and sprains
It is a great remedy for osteoarthrosis due to bruises mechanical injury and sprains dislocation of bones.
It is indicated when there is a sore, lame, bruised feeling over the entire body after a blow, fall, or any sort of mechanical injury, especially of bones and periosteum.
It is a useful remedy when all parts on which the patient lies are painful as if bruised, the patient is restless and changes position quite frequently when lying.
Dosage and potency: 200c potency take 4 globules (pills) twice a day till the improvement occurs.
5. Calcarea Phosphorica – For osteoarthrosis with impaired nutrition
It is a great remedy for osteoarthrosis from defective bone development, there is a tendency to curvature of long bones.
It is indicated for osteoarthrosis arising due to grief, disappointed love, overstudy, unpleasant news, and getting wet.
It is indicated when there is debility remaining after acute diseases, there is numbness in joints.
Dosage and potency: 30c,200c potency of dilution, take 2-3 drops in half cup of water one time a day for 3 days.
6. Calcarea Flourica – For osteoarthrosis with bone spurs
It is a great remedy for osteoarthrosis with a tendency to form calcium spurs and caries in the bones.
It is indicated when there are enlargements of bone with or without caries.
Dosage and potency: 30c, 200c potency, take 2-3 drops of dilution in half cup of water and take twice a day till the improvement.
7. Aurum Metallicum – For osteoarthrosis due to depression or stress
Aurum Metallicum is a useful remedy in osteoarthrosis in old people who are tired of life depressed.
It is indicated when there is profound melancholy and constantly dwelling on suicide, hurried worried and uneasy, and restless.
It is indicated in caries of cranial bones and has violent pains at night.
There is an offensive odor, with a violent pain in bones and extremities.
Dosage and potency: 30c, 200c, 4 globules (pills) twice a day till the improvement is seen.
8. Flouric Acid – For osteoarthrosis due to caries of bones
This remedy is often indicated for osteoarthrosis in which there is calcareous degeneration of the joints.
It is indicated when the osteoarthrosis is in the stage when it causes necrosis of bones there is a lightning type of pain on a small spot, pains come suddenly last for a short time and disappear quickly.
Dosage and potency: – 200c potency, take 4 globules thrice a day up to improvement.
9. Phosphoric Acid – For Osteoarthrosis with great weakness
It is indicated when there is osteoarthrosis due to bad news, grief, sorrow, homesickness, disappointed love, loss of vital fluids, shock, injury, acid drinks- rich food, and fruits.
It is indicated when there is a loss of vital fluids long continued mental grief, there is trembling, and the legs are weak, so stumble easily.
Dosage and potency: 30c, 200c take 3-4 drops of dilution in half a cup of water twice a day.
10. Phosphorus – For Osteoarthrosis restlessness and anxiety
It is a great remedy for Osteoarthrosis occurring from lifting, sprains, and exposure to drenching rains while washing clothes.
It is indicated when the patient suffers from anxiety and feels restless, with a tendency to joint swelling, the patient is constantly moving and cannot sit in one place.
It is indicated when the patient is sensitive, the joints are swollen and inflamed, there is burning in spots, and a weak gone feeling in the stomach.
Dosage and potency: 200c potency, take four globules under the tongue, twice a day for 15 days or until the improvement appears.
Remember that homeopathic remedies are prescribed based on individual symptoms and characteristics. It’s crucial to consult with a qualified homeopath for proper evaluation and personalized treatment. Homeopathy focuses on treating the whole person, so a detailed case study is necessary to select the most appropriate remedy.
Homeopathic medicines should be taken only when prescribed by a homeopathic physician. Self-medication may aggravate the original conditions.
